5/8/25 – 7/14/25
Stevie was born four weeks early on May 8, 2025, in Oakland, California. Weighing in at 6 lbs 8oz, she looked, felt, and acted like a healthy baby girl with a head full of hair, which wasn’t the least bit surprising if you’d met her parents. She had a standard two night hospital stay before getting discharged to go home.
Stevie spent the next few days in the love and care of her exhausted parents and very excited grandparents. She’d sleep, occasionally open her eyes, cry on and off through the night, and watch playoff basketball with her mom and dad.

Things seemed normal, until they weren’t. It started with some heavier breathing that sounded like minor congestion. Then came the difficult feeds, excessive lethargy, and something just feeling “off.” After a handful of hospital visits, Stevie was admitted to the Neonatal Intensive Care Unit (NICU) at 6 days old.
We were overwhelmed with conflicting emotions. On one hand, we were absolutely terrified. We had her at home, in our arms, and now she’s staying overnight at the hospital? What could have happened? Why?
On the other, we reminded ourselves that lots of babies go to the NICU. We even knew a few ourselves, and those kids are doing great now. Plus, she got carted through the hospital in an oversized gurney, leading to so many laughs and smiles from the nurses. How bad could it really be?
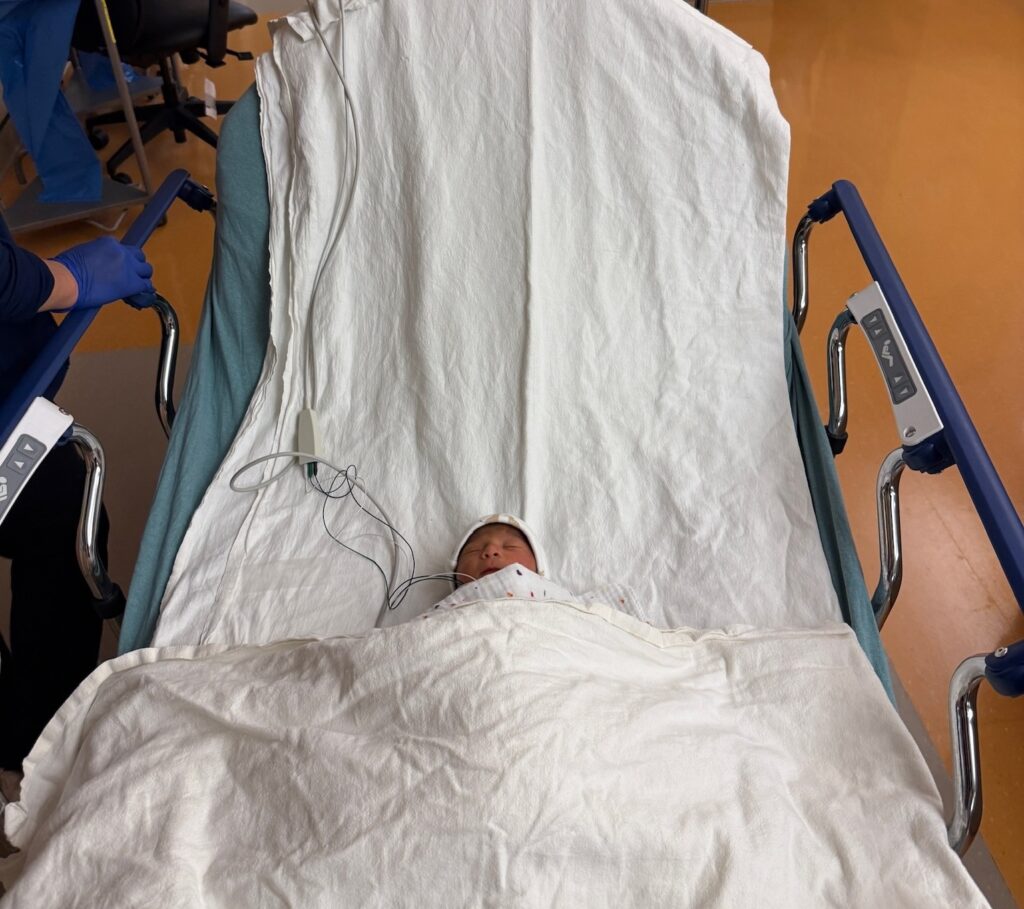
The first 48 hours in the ICU were an onslaught of awful news: unconscionably low platelet counts; high ammonia levels; coagulopathy; seizures. Everything pointed to her liver failing, resulting in an emergency transfer to UCSF, a level IV ICU facility, to figure out whatever the hell was happening.
The physicians worked quickly to stabilize Stevie and assemble her preliminary diagnosis: she was battling a complex combination of enterovirus, acute liver failure, neonatal hemochromatosis, and a form of hemophagocytic lymphohistiocytosis (HLH)—a rare, life-threatening disorder where the immune system overreacts and attacks the body’s own cells and tissues.
To treat this, the doctors would administer immune-suppressing medications and start complete renal replacement therapy (CRRT) to lower her ammonia levels. The hope was that once her inflammation was under control, her liver could regain its functionality.
This all seemed to work, at first. But soon we would realize that the virus, her liver failure, and the increasing issues related to coagulapathy across her other organs were getting more and more difficult to manage. As the weeks accumulated, so did her complications, ultimately leading to her passing.
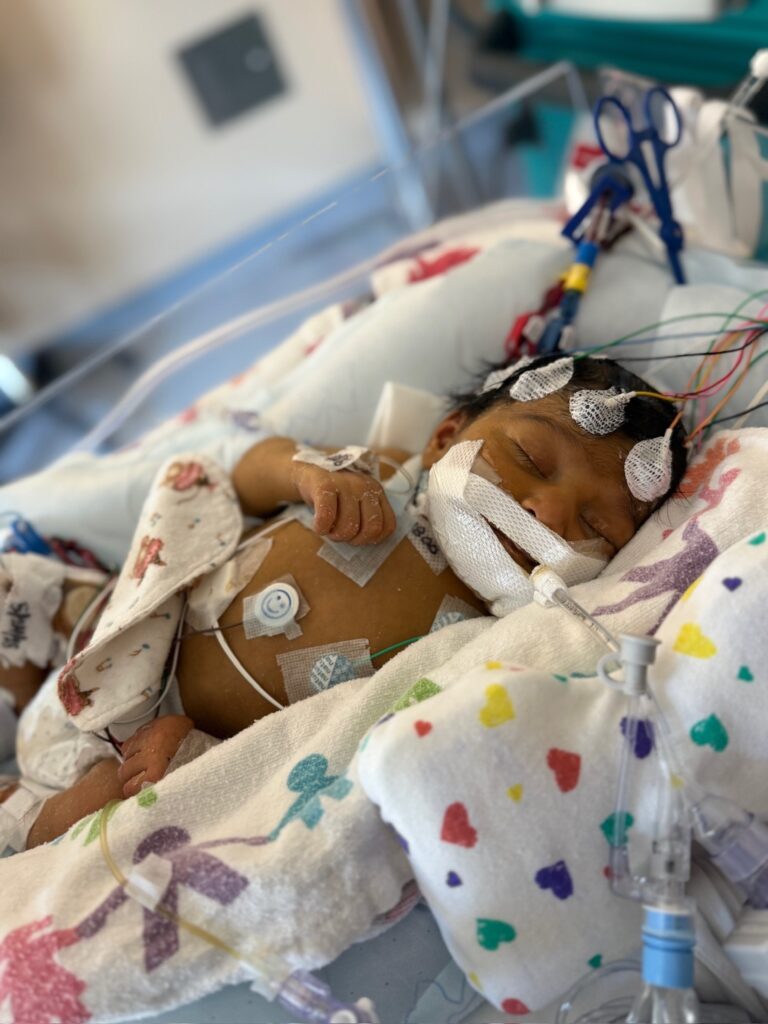
Because Stevie was hooked up to so many wires and supporting machines, we were rarely able to hold her. Each night before we left the hospital, Joli would touch Stevie softly and say, “We’ll hold each other in our hearts.” That line carried us through each emotional evening and continues to be how we stay connected to her to this day.
We’ll always, always hold you in our hearts, Stevie.
*The 8+ weeks we spent with Stevie in the ICU were the most excruciating days of our lives. While it’s difficult (and lengthy) to put this experience into writing, we’re happy to discuss it in more detail, especially with parents or caretakers in a similar situation.